Kronik sinüs enfeksiyonlarının temel nedeni, sinüslerde üretilen mukusun burun içine boşalmasını sağlayan küçük kanalların (ostium) tıkanmasıdır. Bu durum, salgıların sinüs içinde birikmesine ve sinüs havalanmasının bozulması sonucunda sinüslerde enfeksiyon oluşmasına yol açar.
Balon sinoplasti, sinüslerin tıkalı veya daralmış boşalma kanallarının, herhangi bir doku kesilip çıkarılmadan, yalnızca balon yardımıyla genişletilmesi prensibine dayanan bir tekniktir. Bu sayede sinüslerin havalanma ve drenaj fonksiyonları yeniden sağlanır.
Balon Sinoplasti Tekniğinin Avantajları:
Standart endoskopik cerrahi teknikleriyle karşılaştırıldığında balon sinoplastinin önemli avantajları bulunmaktadır:
- Etkili ve güvenli yöntem: Komplikasyon ihtimali oldukça düşüktür. Bu işlem için uygun hastalarda balon ile genişletilen sinüs drenaj kanallarının işlemi takip eden süreçte büyük oranda açık kaldığı izlenmiştir.
- Çok az doku hasarı: Küçük, yumuşak ve elastik ekipmanlar kullanılarak kapalı sinüs drenaj kanalları nazikçe açılır, bu da çok az doku hasarı ile sonuç elde edilmesini sağlar.
- Minimal kanama: İşlem sırasında kanama miktarı oldukça düşüktür.
- Hızlı iyileşme süresi: Çoğu hasta 24 saat içinde normal hayatına dönebilmektedir.
- Diğer tedavileri engellememe: Balon Sinoplastinin aynı bölgede daha sonra yapılabilecek endoskopik cerrahi gibi diğer tedavileri engelleyici bir rolü yoktur.
Balon sinoplasti tek başına kullanılabileceği gibi, özel durumlarda standart endoskopik sinüs cerrahisi ile birlikte de uygulanabilmektedir.
Balon Sinoplasti Hangi Durumlarda Uygulanır?
Burun çevresinde her bir tarafta dörder adet olmak üzere toplam sekiz sinüs bulunur. Bunlar alın kemikleri içinde frontal, yanak kemikleri içinde maksiller, gözler arasında etmoid ve kafanın tam merkezinde en geride yer alan sfenoid sinüslerdir.
Nadir anatomik varyasyonlar dışında frontal, maksiller ve sfenoid sinüsler, burun içine tek bir boşalma kanalı (ostium) ile açılan büyük boşluklardır. Etmoid sinüsler ise çok küçük boşalma kanalları olan, bal peteği gibi 10-15 küçük odacıktan oluşur.
Balon sinoplasti sırasında kullanılan ekipmanların boyutları frontal, maksiller ve sfenoid sinüslerin boşalma kanallarından geçmeye uygunken, etmoid sinüsler için oldukça büyük kalırlar. Bu nedenle, etmoid sinüzit vakaları standart balon sinoplasti tekniği için uygun değildir. Ameliyat gerektiren kronik sinüziti olan hastalarda en fazla hastalık görülen sinüsler etmoid sinüslerdir. Bu sebeple, tüm kronik sinüzit hastaları içinde sadece standart balon sinoplasti tekniği kullanılarak tüm hastalıklı sinüslerine müdahale edilebilecek hastaların oranı nispeten azdır.
Günümüzde yaygın nazal polipleri olan hastalarda sinoplasti kullanımı kısıtlıdır. Bu vakalarda klasik endoskopik cerrahi sırasında belli bölgelerde balon tekniği kullanılabildiği gibi, sadece klasik endoskopik sinüs cerrahisi de tercih edilebilmektedir. Balon sinoplasti tekniği, endoskopik sinüs cerrahisinin yerini tamamen alan bir yöntem olmayıp, özel durumlarda önemli avantajlar sağlayan yardımcı bir teknoloji olarak kabul edilmelidir.
Balon Sinoplasti Güvenli midir?
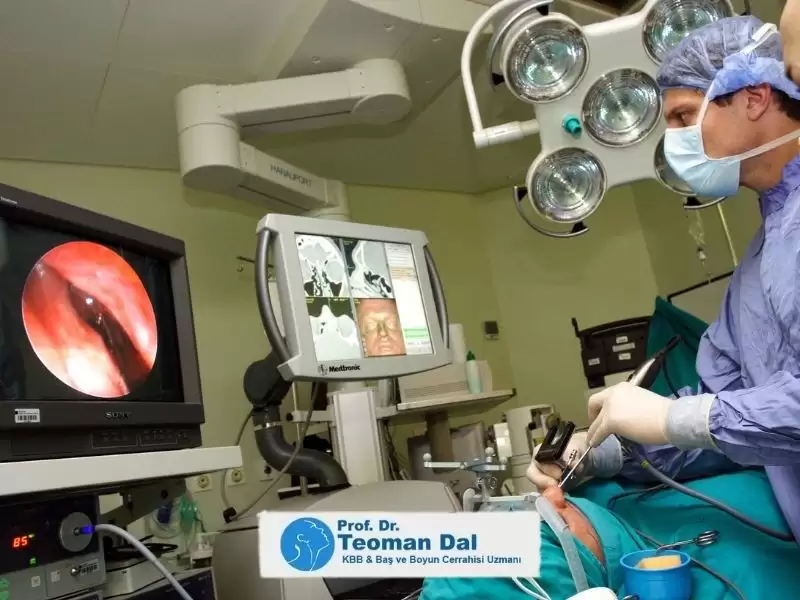
Balon sinoplasti teknolojisi ilk olarak uygulanmaya başlandığında, ameliyat sırasında balon kateterlerin sinüs kanallarında uygun yerleşimini sağlamak için skopi cihazı kullanılması nedeniyle hastaların X ışınına maruz kalmaları önemli bir sorun olarak görülmekteydi. Daha sonra geliştirilen ışıklı kılavuz tellerin kullanıma girmesiyle, alın ve yanak sinüslerine skopi kullanılmadan girilebilme imkanının sağlanması bu problemi önemli ölçüde çözmüştür.
Bugün için balon sinoplasti sırasında yalnızca sinüs içindeki ışığın dışarıdan görülmesinin mümkün olmadığı en gerideki sfenoid sinüslere müdahale ederken X ışını veren skopi cihazı kullanılmaktadır. Skopi cihazında gereken ayarların yapılmasının yanı sıra, ameliyatın tecrübeli bir uzman tarafından uygun teknik kullanılarak oldukça kısa sürmesi, işlem sırasında hastaya verilen X ışını miktarının son derece az olmasını sağlamaktadır.
Balon sinoplasti tekniği kullanılan ameliyatlarda bugüne kadar çok az sayıda komplikasyon rapor edilmiştir. Bu komplikasyonlar içinde en önemlisi, alın sinüsü boşalma kanalının balon ile genişletilmesi sırasında hemen komşuluğunda kafa kaidesinde hasar oluşmasıdır.