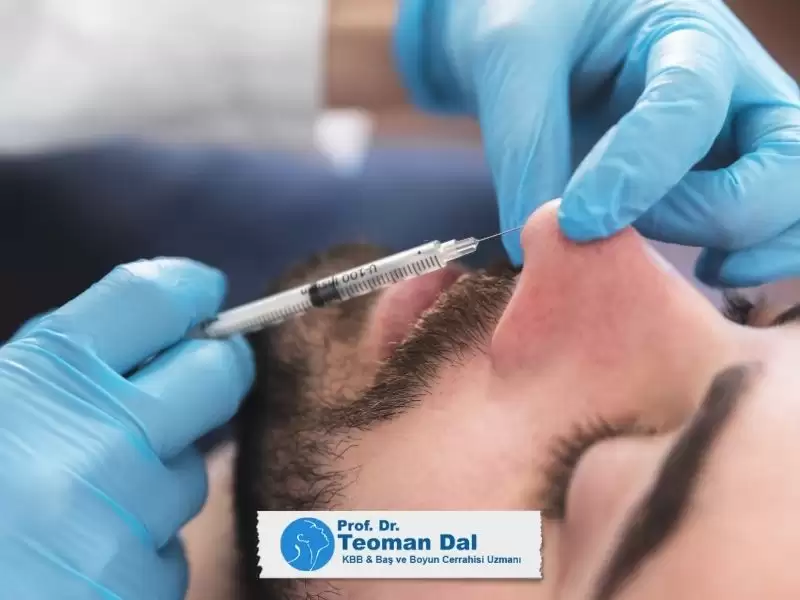
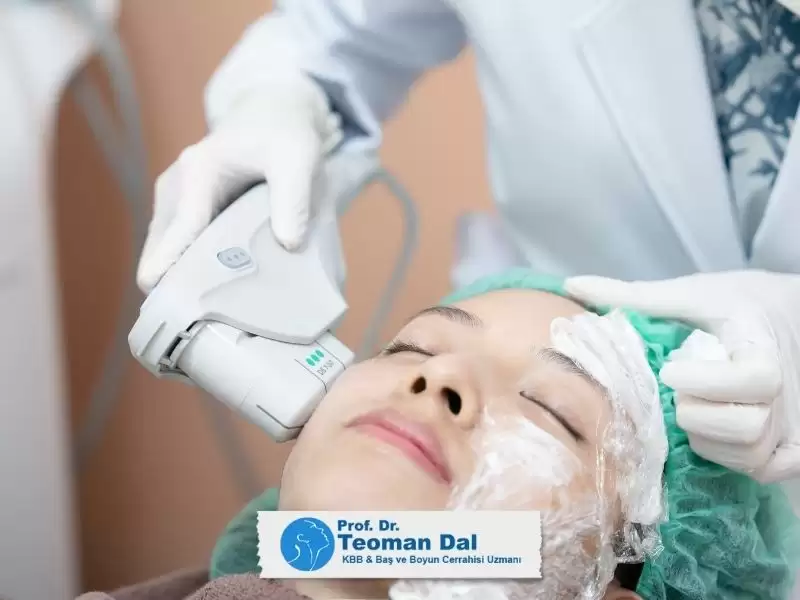
“Fasial plastik cerrahi”, “Yüz plastik cerrahisi” ya da “Yüz Estetik Cerrahisi” kulak burun boğaz uzmanlık alanının alt uzmanlık dallarından birisidir. Yüz, baş ve boyun bölgesindeki bütün anatomik yapılar üzerinde kozmetik veya onarım (rekonstrüksiyon) amaçlı yapılan tüm cerrahi müdahaleler yüz plastik cerrahisi uzmanlık alanının kapsamına girmektedir.
Yüz plastik cerrahisinin kapsadığı konular şu şekildedir:
I. Estetik - Kozmetik
- Rinoplasti
- Septorinoplasti
- Göz kapağı ameliyatları - Blefaroplasti
- Yüz germe (face lift)
- Boyun germe (Necklift)
- Çene ucu estetiği - Mentoplasti (augmentasyon, redüksiyon)
- Yanak implantları - Malar implant
- Alın germe - Koronal / frontal lift
- Kaş kaldırma
- Servikofasiyal liposuction
- Cilt soyma - Dermabrazyon
- Kimyasal peeling, lazer resurfacing
- Saç ekimi (Flep, deri azaltma, mikro, mini veya punch greft)
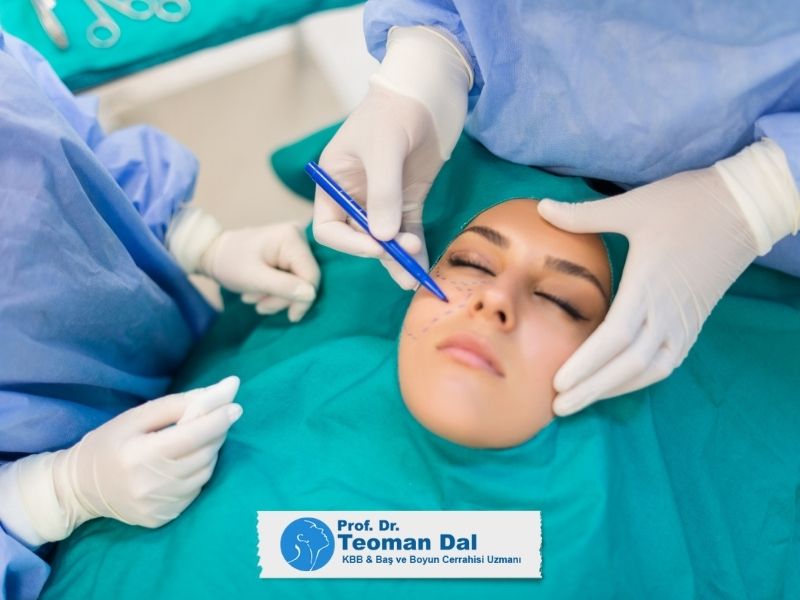
II.Onarım - Rekonstrüktif
- Alt çene kemiği - Mandibula rekonstrüksiyonu
- Yüz kemikleri greftlemesi /rekonstrüksiyonu
- Ortognatik müdaheleler
- Greftler (kısmi, tam, kompozit, cilt, cilt-yağ)
- Flepler (lokal, bölgesel, distal, serbest)
- Yüz siniri - Fasiyal sinir rekonstrüksiyonu (sinir greftleri, kas sling, diğer)
- Yara izi - Skar revizyonu (Z-plasti, W-plasti, geometrik kesik çizgi kapatma, kompleks diğer, tüm yüz dermabrazyon)
- Kompleks septoplasti
- Major burun rekonstrüksiyonu
- Major kulak rekonstrüksiyonu
- Göz kağağı onarımları - Palpebra / perioküler rekonstrüksiyon
- Doku genişleticiler
- Mohs cerrahisi
III. Travma
- Yaygın yumuşak doku onarımı
- Fasiyal sinir onarımı
- Göz yaşı sistemi - Lakrimal onarım
- Yüz kemikleri kırıkları (frontal, midfasiyal, nazal, malar, orbital, mandibüler)
IV. Doğumsal – Konjenital Anomaliler
- Major hemanjiom / lenfanjiom (rezeksiyon, tedavi)
- Koanal atrezi onarımı
- Yarık dudak (tek taraflı, çift taraflı)
- Alveolar yarık onarımı
- Yarık damak onarımı
- Kulak kepçesi gelişmemesi - Mikrotia rekonstrüksiyonu
- Kepçe kulak estetiği - Otoplasti
- Diğer estetik kulak kepçesi ameliyatları
V. Baş Boyun Cerrahisi
- Tükürük bezi ameliyatları
- Dudak kanserleri
- Üst çene (maksilla) kanserleri
- Alt çene (mandibula) kanserleri
- Dil kanseri ameliyatı
- Burun cildi tümörleri
- Kulak kepçesi tümörleri
- Boyun diseksiyonu