İçindekiler
- Horlama ve Uyku Apnesi Hakkında Bilmeniz Gerekenler
- Uyku Apnesi Belirtileri Nelerdir?
- Gece Görülen Uyku Apnesi Belirtileri
- Gündüz Görülen Uyku Apnesi Belirtileri
- Uyku Apnesi Kimlerde Daha Sık Görülür?
- Uyku Apnesi Nasıl Teşhis Edilir?
- Uyku Apnesi Tanısında Kullanılan Yöntemler
- Uyku Apnesi Nasıl Tedavi Edilir?
Horlama ve Uyku Apnesi Hakkında Bilmeniz Gerekenler
Horlama, genellikle uyku sırasında üst solunum yolunun daralması sonucu hava akımının titreşim yaratmasıyla oluşan sesli bir durumdur. Özellikle boğaz çevresindeki yumuşak dokuların gevşemesiyle birlikte bu titreşim artar. Horlama tek başına görülebileceği gibi, daha ciddi bir sağlık sorunu olan obstrüktif uyku apnesi sendromu (OSAS) ile birlikte de ortaya çıkabilir.
Uyku apnesi, kişinin uyku sırasında solunumunun geçici olarak durmasıdır. Bu duraklamalar 10 saniyeden uzun sürebilir ve gece boyunca onlarca kez tekrar edebilir. Apne sırasında vücuda yeterli oksijen gitmez, bu da kalp-damar sağlığını olumsuz etkileyebilir.
Uyku apnesi tipleri:
- Basit Horlama: Solunum durması olmadan, sadece sesli horlama ile seyreden durumdur.
- Üst Solunum Yolu Direnç Sendromu: Solunum durmaz ama hava akımı kısıtlanır ve uyku bölünür.
- Obstrüktif Uyku Apnesi: Solunum yollarının tamamen ya da kısmen kapanması sonucu apne veya hipopne atakları görülür.
Uyku Apnesi Belirtileri Nelerdir?
Uyku apnesi, genellikle fark edilmeden ilerleyen ve ciddi sağlık sorunlarına yol açabilen bir uyku bozukluğudur. Belirtiler hem gece hem de gündüz görülebilir ve hastalığın şiddetine göre değişkenlik gösterebilir.
Gece Görülen Uyku Apnesi Belirtileri
- Yüksek sesle horlama: Uyku apnesinin en yaygın ve erken belirtilerindendir. Horlama aralıklı olabilir ve apne atakları sırasında durabilir.
- Solunum durması veya boğulma hissi: Uyku sırasında solunumun 10 saniyeden uzun süreyle kesilmesi (apne), ardından ani nefes alma ve boğulma hissi görülebilir.
- Sık sık uyanma: Kaliteli uyku bölünür, kişi gece boyunca defalarca uyanabilir.
- Gece terlemesi: Uyku sırasında gövde ve ense bölgesinde yoğun terleme olabilir.
- Sık idrara kalkma: Uyku apnesi olan kişiler gece boyunca birden fazla kez tuvalete gitme ihtiyacı hissedebilir.
Gündüz Görülen Uyku Apnesi Belirtileri
- Sabah yorgunluğu ve baş ağrısı: Uyandığınızda dinlenmemiş hissetmek ve baş ağrısı yaşamak sık rastlanan belirtilerdir.
- Aşırı gündüz uykululuğu: Gün içinde uyuklama, özellikle toplantılarda, konuşurken ya da araba kullanırken bile uykuya dalma eğilimi olabilir.
- Konsantrasyon ve hafıza problemleri: Dikkat dağınıklığı, unutkanlık ve odaklanma güçlüğü yaşanabilir.
- Huzursuzluk, sinirlilik ve depresyon belirtileri: Uyku kalitesinin düşmesi psikolojik durumu da etkiler.
- Cinsel istekte azalma: Hormonal düzensizliklere bağlı olarak libido düşüklüğü görülebilir.
Uyku Apnesi Kimlerde Daha Sık Görülür?
- Kilolu bireyler
- Kalın boyun çevresi olan kişiler (erkeklerde 43 cm+, kadınlarda 38 cm+)
- Orta yaş ve üzeri erkekler
- Alkol veya yatıştırıcı ilaç kullananlar
- Burun tıkanıklığı veya çene yapısında bozukluk olanlar
Uyku Apnesi Nasıl Teşhis Edilir?
Uyku apnesi hastalığının teşhisi, yalnızca belirtilere bakarak konulamaz. Bu nedenle hem fiziksel muayene hem de bazı ileri tetkik yöntemleri gereklidir. Uyku apnesi tanısı koymak için en güvenilir yöntem ise polisomnografi, yani uyku testidir.
Uyku Apnesi Tanısında Kullanılan Yöntemler
1. Tıbbi Öykü ve Şikâyetlerin Değerlendirilmesi
Hasta ile yapılan görüşmede, horlama, gündüz uykululuk hali, sabah yorgunluğu, gece nefes kesilmesi gibi şikayetler sorgulanır. Ayrıca hastanın eşinden veya birlikte uyuyan kişiden alınan bilgiler tanı açısından çok değerlidir.
2. Fiziksel Muayene
- Vücut kitle indeksi (BMI) ve boyun çevresi ölçülür.
- Ağız, boğaz ve burun yolları detaylı incelenir.
- Çene yapısı, dilin pozisyonu, bademcik büyüklüğü değerlendirilir.
3. Kulak Burun Boğaz (KBB) Muayenesi
KBB uzmanı, burun tıkanıklığı, yumuşak damak yapısı ve üst solunum yollarındaki darlıkları değerlendirir. Endoskopik muayene ile dil kökü ve geniz bölgesi gibi derin anatomik yapılar da görüntülenebilir.

4. Radyolojik Görüntüleme
- Bilgisayarlı tomografi (BT) ve Manyetik Rezonans (MR) ile üst solunum yollarındaki darlıklar ve çene-yüz yapısı detaylı incelenebilir.
- Sefalometrik analiz, cerrahi planlamalarda kullanılır.
5. Uyku Testi (Polisomnografi)
Uyku apnesi teşhisinde altın standarttır. Uyku sırasında şu veriler ölçülür:
- Solunum durması (apne) sayısı ve süresi
- Oksijen seviyesi (O2 satürasyonu)
- Kalp ritmi
- Horlama sesi
- Uyku evreleri ve beyin aktiviteleri
Apne-Hipopne İndeksi (AHİ) olarak adlandırılan değer ile hastalığın şiddeti belirlenir:
- AHİ 5–15: Hafif uyku apnesi
- AHİ 15–30: Orta derece uyku apnesi
- AHİ 30+: Ciddi uyku apnesi
6. Uyku Endoskopisi
Hafif anestezi altında yapılan bu özel endoskopi yöntemiyle hastanın gerçek uyku haline benzer bir durumda solunum yollarındaki tıkanıklıklar değerlendirilir. Cerrahi tedavi planlamasında oldukça faydalıdır.
Uyku Apnesi Nasıl Tedavi Edilir?
Uyku apnesi tedavisi, hastalığın şiddetine, altta yatan nedenlere ve hastanın genel sağlık durumuna göre planlanır. Tedavi yöntemleri üç ana grupta incelenir: genel önlemler, özel tedavi yöntemleri ve cerrahi müdahaleler.
1. Genel Önlemler
Uyku apnesi olan birçok kişide yaşam tarzı değişiklikleri tedavinin temelini oluşturur.
Kilo Vermek
Fazla kilo, özellikle boyun ve üst solunum yolu çevresinde yumuşak doku birikimine neden olur. Bu da solunum yolunun daralmasına ve apne ataklarına yol açar. Kilo kaybı hem horlamayı hem de apne şiddetini azaltabilir.
Alkol ve Uyku İlaçlarından Kaçınmak
Yatmadan önce alkol ya da yatıştırıcı ilaç kullanımı, solunum kaslarını gevşeterek apne ataklarını artırabilir. Bu tür maddelerden uzak durmak önerilir.
Uyku Pozisyonunu Değiştirmek
Sırt üstü uyumak, dilin ve yumuşak damağın geriye kaymasına neden olur. Yan yatmak, hava yolunun açık kalmasına yardımcı olur. Bu amaçla özel yastıklar veya pozisyon eğitici aparatlar kullanılabilir.
Burun Tıkanıklığını Gidermek
Burun tıkanıklığı, hava yolundaki direnç artışına sebep olur. Alerji, sinüzit gibi durumların tedavisi veya burun içi yapısal sorunların düzeltilmesi, tedavinin başarısını artırır.
2. Özel Tedavi Yöntemleri
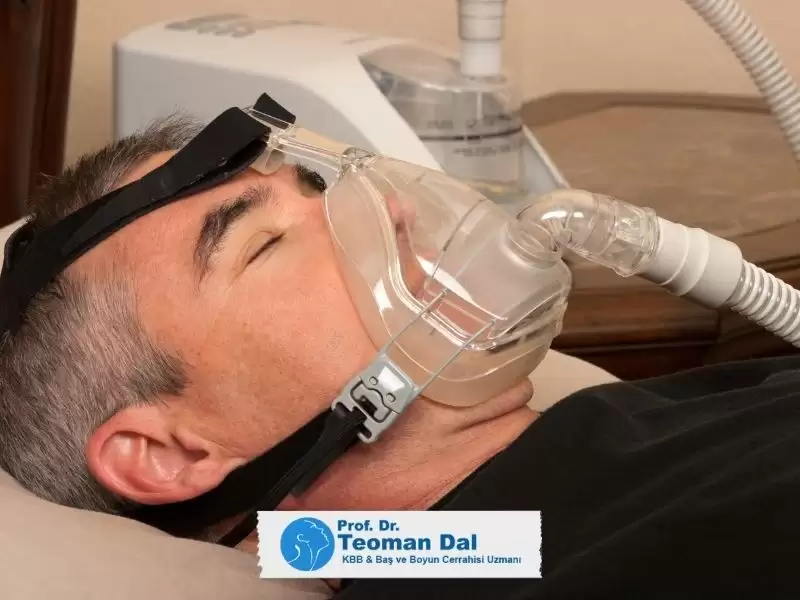
CPAP Cihazı (Sürekli Pozitif Hava Basıncı)
CPAP (Continuous Positive Airway Pressure) cihazı, burun yoluyla pozitif hava basıncı vererek üst solunum yollarının kapanmasını engeller. Uyku apnesi tedavisinde cerrahi dışı en etkili yöntemdir.
- Cihazın her gece düzenli kullanılması gerekir.
- Burun tıkanıklığı olan hastalarda kullanım zor olabilir.
- Bazı hastalarda BPAP gibi çift basınçlı versiyonlar tercih edilir.
Ağız İçi Apareyler
Dili veya alt çeneyi öne iterek hava yolunu açan bu apareyler, özellikle basit horlama ve hafif uyku apnesi olan hastalarda etkili olabilir.
- Diş hekimi kontrolünde uygulanmalıdır.
- Uzun süreli kullanımda çene ve diş problemleri gelişebilir.
İlaç Tedavisi
Uyku apnesi için etkili bir ilaç tedavisi bulunmamakla birlikte; bazı özel durumlarda REM uykusunu baskılayan veya kas tonusunu artıran ilaçlar kullanılabilir. Sadece doktor kontrolünde verilmelidir.
3. Cerrahi Tedavi Seçenekleri
Eğer hava yolunda tıkanmaya neden olan anatomik problemler varsa, cerrahi tedavi gündeme gelir. Aşağıdaki durumlarda cerrahi düşünülebilir:
- Apne hipopne indeksi (AHİ) 20’nin üzerinde ise
- Kan oksijen düzeyi %90’ın altına düşüyorsa
- CPAP kullanımına uyum sağlanamıyorsa
Başlıca Uyku Apnesi Ameliyatları:
- Burun ameliyatları (deviasyon, burun eti küçültme)
- Yumuşak damak ve küçük dil operasyonları (uvulopalatofaringoplasti)
- Dil kökü küçültme ameliyatları
- Çene kemiklerinin ilerletilmesi (maksillomandibular ilerletme)
- Hipoglossal sinir stimülasyonu (dil kaslarını uyarma cihazları)
- Trakeotomi (nadir, çok ileri vakalarda)
Cerrahi kararlar, Polisomnografi, uyku endoskopisi ve diğer görüntüleme yöntemleriyle detaylı değerlendirme sonrası verilmelidir.